
So it’s only natural to assume that a provider will have different responses for different individuals from different states. 
As we all know, insurance companies seem to make decisions by throwing darts at a dartboard. 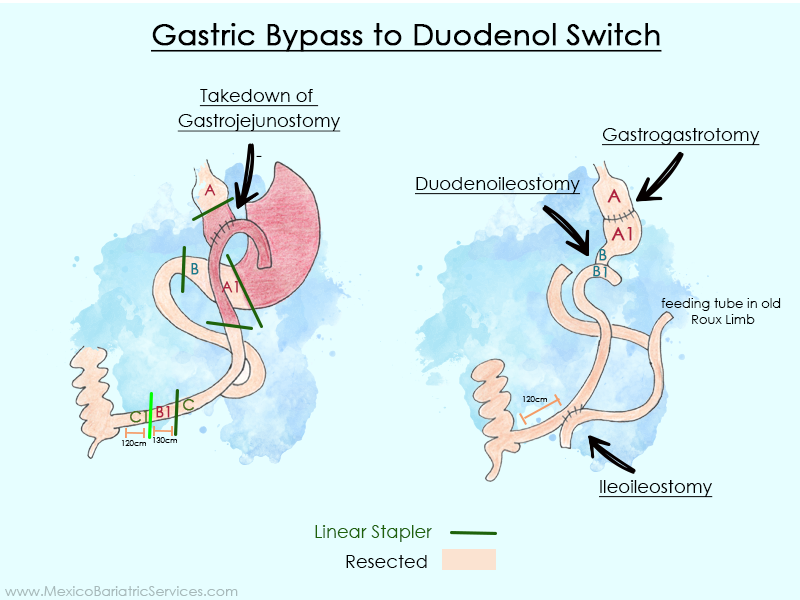
This is a simple question, but a not so simple response. Will My Insurance Provider Cover a Revision? A patient will be dealing with either a revision of a failed bariatric procedure or a revision to a new type of procedure not approved or even in existence at the time of the original surgery. There are several areas where revisions can arise. Revision, defined, is to change or modify (for our purposes, it is to change or modify a prior bariatric surgery). And that word, revision, gives rise to a number of included terms such as failed surgery, non-compliance, and revision to a new procedure. In this article, we’ll talk solely about revisions. Be it plastic surgery, or a revision, the sheer numbers of post-op patients is increasing the demand for these two types of post-op procedures. As a result, I find myself being asked more and more questions regarding post-operative surgery. The weight-loss surgery field experienced exponential growth throughout the past four years.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
